Who is a good candidate for partial knee replacement
There are three main sections in the knee–we refer to them as compartments–that can undergo osteoarthritic changes and these include the inside of the knee, which is more common (the medial compartment), the outside of the knee (the lateral compartment), and underneath the knee cap (patellofemoral joint).
Some patients will have isolated single compartment disease. Approximately 5-10% of patients indicated for knee replacement surgery will undergo replacement of a single compartment, which is known as uni-compartment knee arthroplasty.
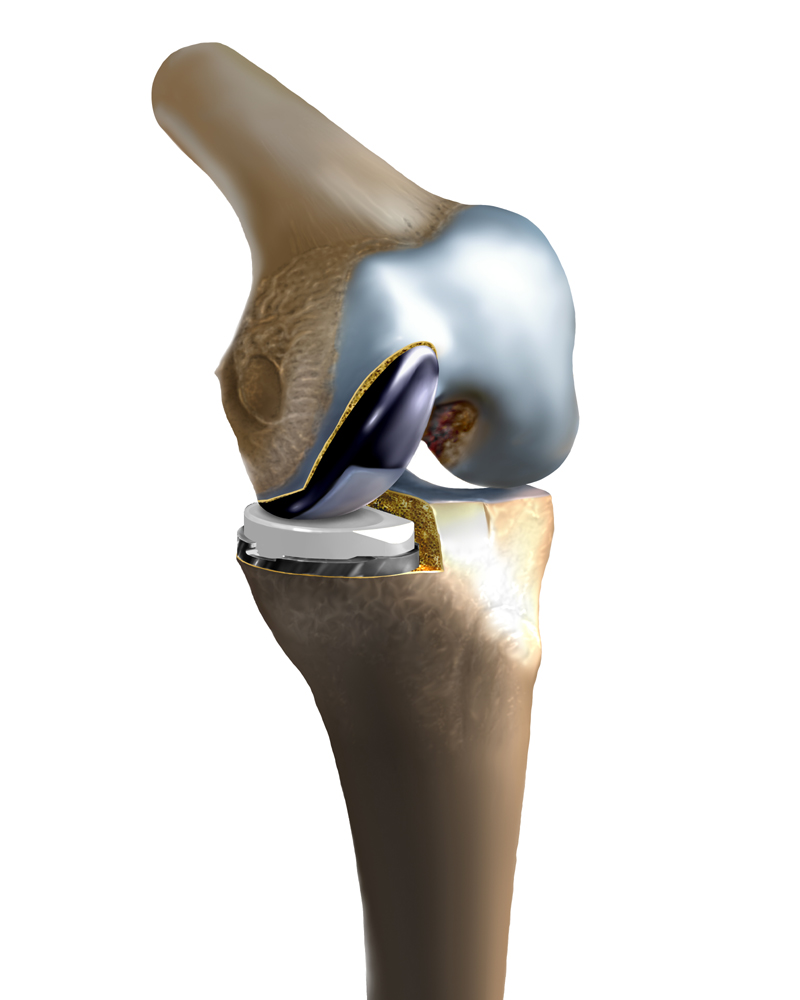
The most common compartment replaced is the medial compartment. Patients typically have osteoarthritis symptoms of stiffness, joint line pain with prolonged activity or standing on the inside of their knee joints, and sometimes they notice progressive bow-legged deformities or prominent bone spur formation. They will typically not complain of pain on the outside of their knee or underneath the kneecap.
This typical patient may be a candidate for partial knee replacement if all conservative, non-operative treatment has failed such as cortisone injections, anti-inflammatories, physical therapy, and even failed arthroscopic surgery.
Out with the old
In the past, patients with these isolated symptoms used to be treated with a joint offloading surgery called high-tibial osteotomy. This required the surgeon to cut the tibia at an angle to remove or open a wedge of bone and place a plate and screws to change the mechanical alignment of the limb to decrease the force on the affected compartment.
However, this procedure required the patient to be non-weight bearing, and sometimes, there would be problems healing the bone in this area, loss of fixation, painful hardware, and problems with the knee-cap tracking and scarring. Over time, this has lost favor for younger and middle age patients in favor of unicompartmental knee replacements, which have improved in design over the decades and have been shown to be effective as a long lasting treatment option.
In with the new
The literature has shown that in the right group of patients with isolated knee osteoarthritis, partial knee replacements can be very effective in alleviating pain from arthritis while lasting 2 or more decades long term. They have been shown to result in quicker recovery, less bleeding, lower complications and provide a more natural feeling and better dynamics than a traditional total knee replacement in many cases.
We are also finding that the old indications are being expanded to incorporate more patients because the results have been more favorable than previously thought. Surgeons who perform a good number of these technically demanding surgeries have become so well trained that many of them are doing these as an outpatient procedure, which I believe is the way of the future.
Occasionally, patients will develop progressive arthritis in other compartments of the knee as a result of the natural progression of the disease. In these cases, if the patient has a partial knee replacement, the revision is much easier to convert the knee to a total knee arthroplasty which is a technical advantage to the joint arthroplasty surgeon.
I believe that if the right patient has isolated osteoarthritic disease this is an excellent option to return them back to their activities and alleviate their pain in the short and long term.
Images provided by:
Smith and Nephew


